| Journal of Medical Cases, ISSN 1923-4155 print, 1923-4163 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Med Cases and Elmer Press Inc |
| Journal website https://jmc.elmerpub.com |
Case Report
Volume 16, Number 3, March 2025, pages 120-126
Lipomatous Hypertrophy of the Interatrial Septum
Adam Goldaa, b , Beata Bialkowska-Niepona,
Tadeusz Zebika
aDepartment of Cardiology, Gliwice Municipal Hospital No. 4, ul. Kosciuszki 29, 44-100
Gliwice, Poland
bCorresponding Author: Adam Golda, Department of Cardiology,
Gliwice Municipal Hospital No. 4, ul. Kosciuszki 29, 44-100 Gliwice, Poland
Manuscript submitted January 14, 2025, accepted March 12, 2025, published online March 25,
2025
Short title: LHIS
doi: https://doi.org/10.14740/jmc5108
| Abstract | ▴Top |
The abnormal accumulation of lipid-rich adipose tissue within the interatrial septum (IAS) is the hallmark of lipomatous hypertrophy of the interatrial septum (LHIS), a relatively rare medical condition. To accurately distinguish LHIS, it is essential to recognize the characteristic “dumbbell” shape of IAS. Here, we present a case of a 59-year-old woman who was suspected of having cardiac myxoma and was subsequently admitted to our hospital. Transthoracic echocardiography of the patient showed that the IAS had a lack of thickening in the region of the foramen ovale and a hyperechogenic structure in the basal and vault portions of IAS. An abnormal mass located in the IAS anterior to the foramen ovale and not infiltrating the foramen ovale was discovered by computed tomography (CT) scan of the heart. The cardiac magnetic resonance imaging (MRI) confirmed the presence of significant fat deposition within the IAS with sparing of the fossa ovalis, which was consistent with the initial findings. The patient was discharged home with the recommendation of regular visits to the cardiology outpatient clinic for LHIS monitoring. The article presents the visualization of LHIS in consecutive diagnostic modalities, summarizes the actual knowledge of LHIS, and enables proper LHIS diagnosis in patients based on available imaging methods.
Keywords: Lipomatous hypertrophy of the interatrial septum; Septal hypertrophy; Abnormal atrial mass; Pseudomasses; Cardiac tumor differential diagnosis
| Introduction | ▴Top |
Lipomatous hypertrophy of the interatrial septum, commonly abbreviated as LHIS, represents a rather uncommon medical condition that is known to influence approximately 2.2% of the population of patients who underwent the computed tomography (CT) scan, with a notable prevalence among elderly, obese patients, and women compared to their male counterparts [1]. Also, there are suggestions that prolonged parenteral nutrition can induce LHIS [2]. It is an underdiagnosed disease, having in mind the quantities of performed cardiac visualization procedures. It has potentially important implications for the patients, the treating physicians, and surgeons that should be taken into account while planning and conducting both the open and the percutaneous procedures within the heart. A better understanding of this disease will ensure adequate treatment because LHIS presents a kind of cardiac tumor that needs a proper differential diagnosis.
LHIS is characterized by the abnormal accumulation of lipid-rich adipose tissue specifically located within the interatrial septum (IAS), causing extensive thickening of the IAS and leading to potential complications in cardiac function such as arrhythmias and hemodynamic obstruction. LHIS, which is classified as a histologically benign neoplasm, represents an abnormal growth wherein an adipose tissue that is typically found within the atrial septum becomes infiltrated with an excessive number of myocardial fibers, resulting in a significant thickening that measures greater than 2 cm, on average 3 cm, up to 6 cm or more [1]. The infiltrating fat is observed to encroach upon the IAS both in the cephalad direction as well as in the caudal direction relative to the fossa ovalis; however, it is important to note that the fossa itself is invariably spared from this infiltration [3]. The characteristic “dumbbell” shape of the IAS is crucial to accurately differentiate LHIS from other types of cardiac tumors, which may include but are not limited to lipoma, myxoma, fibroma, fibroelastoma, rhabdomyoma, liposarcoma, and metastatic lesions that originate from distant sites.
In recent years, the incorporation of advanced non-invasive imaging techniques into routine diagnostic procedures has greatly enhanced the ability to observe LHIS in living patients, employing modalities such as echocardiography (Echo), CT, magnetic resonance imaging (MRI), and positron emission tomography (PET), which collectively contribute to a more comprehensive understanding of this rare cardiac condition and its implications for patient care.
The objective of our article was to present a case report of a 59-year-old woman referred to our department with a suspicion of a cardiac tumor within the IAS and summarize the available knowledge of this disease.
| Case Report | ▴Top |
Investigations
A 59-year-old asymptomatic woman was sent to the hospital with the suspicion of cardiac myxoma after a screening Echo for a cardiac function in the outpatient clinic. She had a history of arterial hypertension treated sufficiently with ramipril 5 mg b.i.d., and hypercholesterolemia treated with atorvastatin 20 mg once a day. Her medical history was positive for nicotine addiction and she smoked combustible cigarettes. The family history of cardiovascular diseases was unremarkable. Two months prior to the admission to the hospital, the patient had an Echo as a part of routine examination in her outpatient clinic, which revealed accidentally a double thickening of the IAS, with a good systolic function of the heart, no signs of right ventricle overload, and no significant disease of the cardiac valves.
Diagnosis
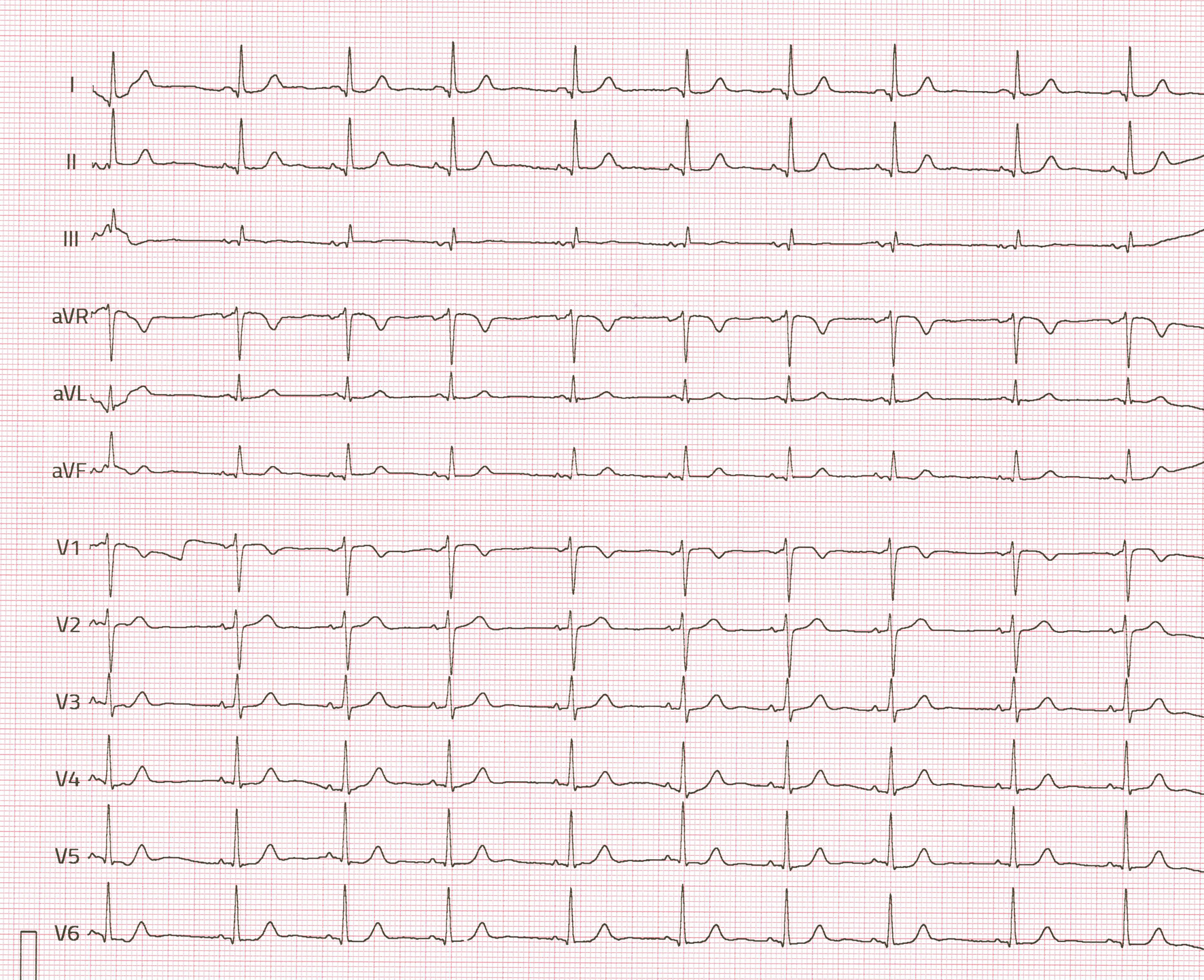
The laboratory test showed no abnormalities in blood count, creatinine, electrolytes, and C-reactive protein values. The 12-lead electrocardiography (ECG) revealed a sinus rhythm of 60/min, intermediate heart axis, and the QRS complex within normal limits (Fig. 1). The transthoracic echocardiography (TTE) repeated at admission to the hospital revealed a normal dimension of the heart with the proper function of both ventricles, trivial mitral insufficiency, and normal function of the other cardiac valves. The selected scan of the TTE is presented in Figure 2. However, the atrial septum had a hyperechogenic structure in the basal and vault parts with a distinct thickening of the septum primum and the secundum adjacent to the fossa ovalis. The findings were confirmed in transesophageal echocardiography (TEE). The patient was referred for a CT scan of the heart, which revealed an abnormal mass area of density of lipomatous tissue (about 50 Hounsfield units) localized in the IAS anterior to the foramen ovale and not infiltrating the foramen ovale with 31 × 21 mm dimension. The abnormal mass had no visible capsule and poured off with the intracardiac lipomatous tissue. There were also signs of modeling of the right atrium and the lower part of the right superior vena cava. Apart from that, the heart and great vessel CT scan was without detectable pathologies. The CT scan confirmed the suspicion of LHIS. The selected scan of the patient’s CT of the heart is presented in Figure 3. The patient was referred for further evaluation to MRI for a more detailed analysis. This imaging modality would allow for a comprehensive assessment of the cardiac structures and any potential implications of the observed lipomatous changes. The examination confirmed the good systolic function of both ventricles with no signs of cardiac oedema and discrete, post-inflammatory bands of subepicardial enhancement in the anterior basal segment as well as the septal and inferior middle segments. The presence of significant fat deposition within the IAS with sparing of the fossa ovalis was consistent with the initial findings. Further evaluation revealed no associated functional impairment or obstruction, suggesting that while the lipomatous hypertrophy was notable, it did not pose an immediate risk to the patient’s cardiac function. The selected scan of the patient’s cardiac MRI is presented in Figure 4.
 Click for large image |
Figure 1. Electrocardiography (ECG) recording of the patient with lipomatous hypertrophy of interatrial septum (LHIS). |
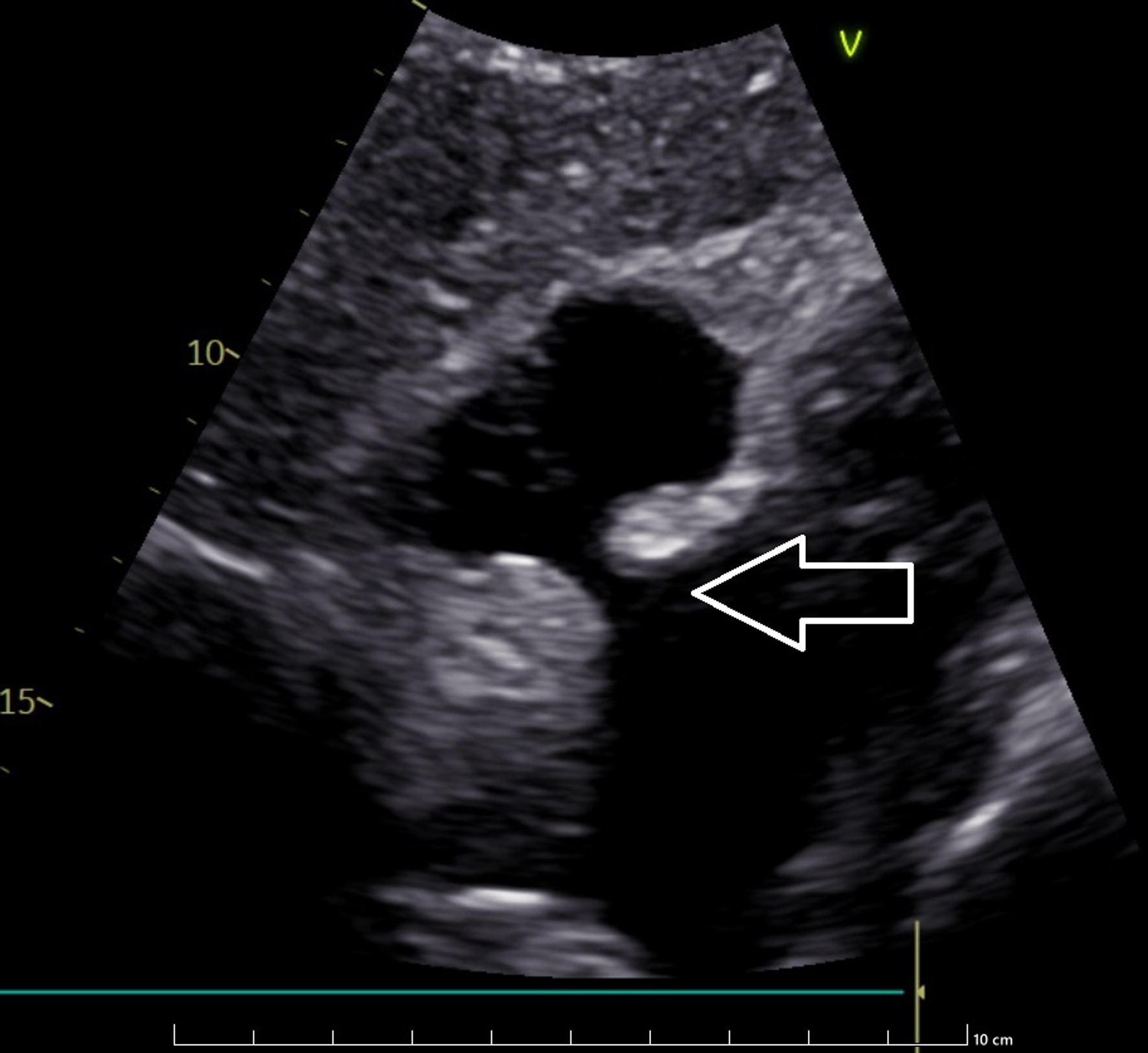 Click for large image |
Figure 2. Modified substernal projection presenting “dumbbell” shape of echo intense acoustic shadow in echocardiography. The arrow indicates the interatrial thickening. |
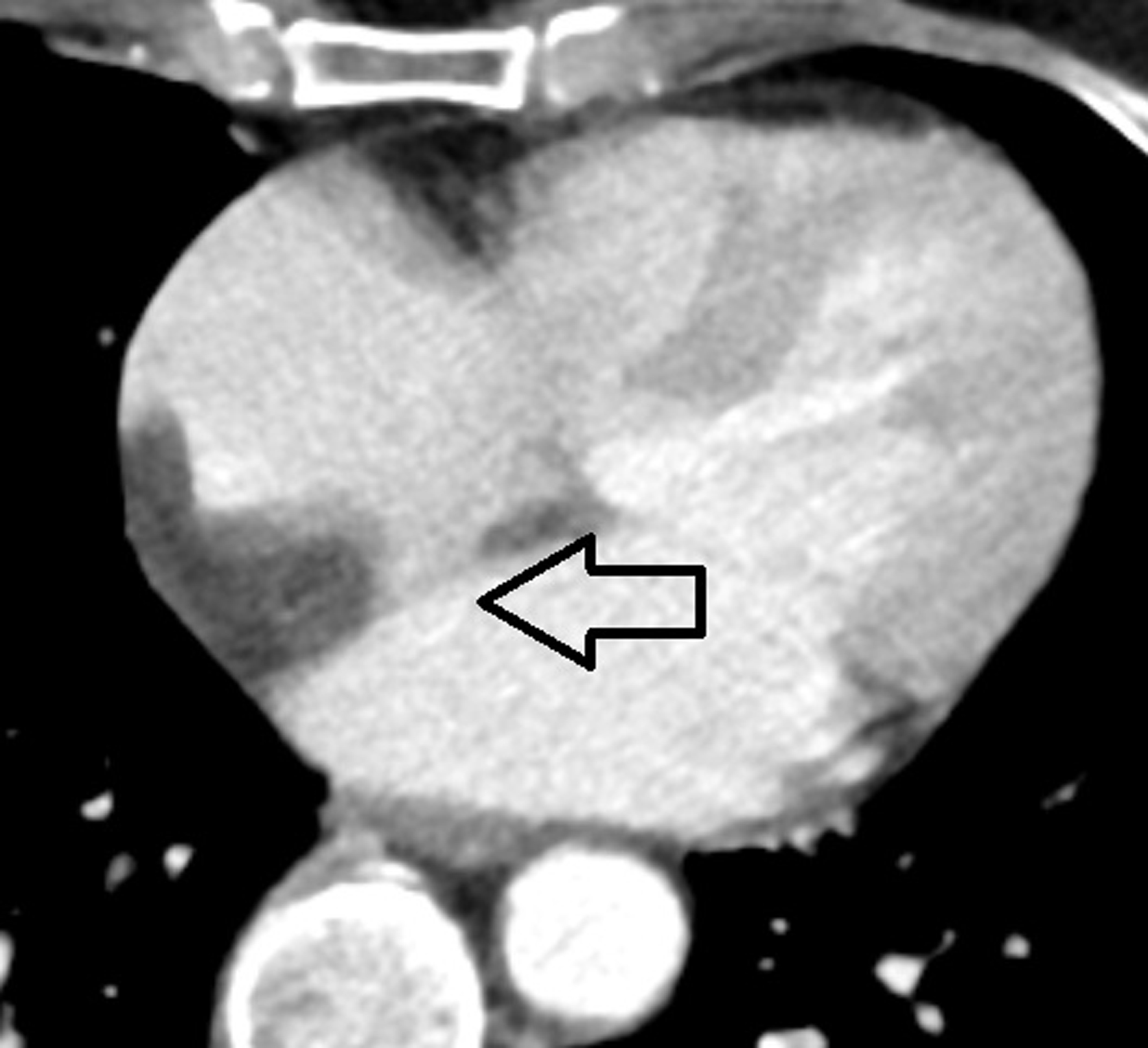 Click for large image |
Figure 3. Contrast-enhanced computed tomography of the heart. The arrow indicates the interatrial thickening. |
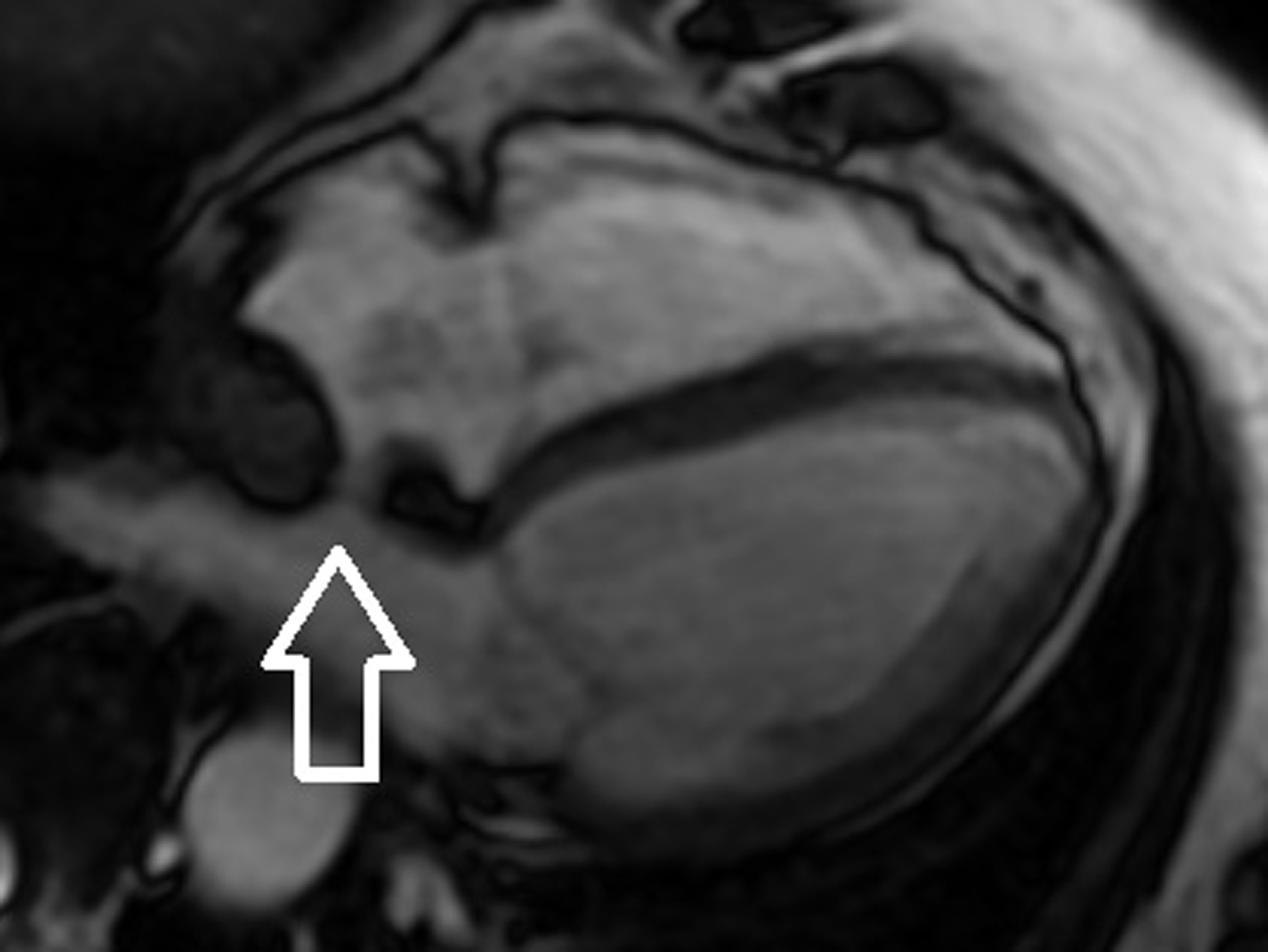 Click for large image |
Figure 4. Contrast-enhanced magnetic resonance imaging. The arrow indicates the interatrial thickening visible in the modified four-chamber view. |
Treatment
The patient was qualified for conservative treatment of LHIS due to no signs of blood flow obstruction within the heart and no information on eventual heart rhythm disturbances. She was instructed on the need to quit smoking, and the medication regimen was modified to telmisartan 80 mg once a day, lercanidipine 10 mg once a day, and atorvastatin 40 mg once a day. The patient was discharged from the hospital in good condition and was referred to ambulatory cardiovascular care.
Follow-up
Follow-up appointments were scheduled to monitor her, ensure adherence to the new treatment, and monitor the LHIS size and the hemodynamic status.
| Discussion | ▴Top |
In this report, we present a rare case of LHIS. The abnormal mass within the IAS was discovered accidentally during a routine Echo in the outpatient clinic and was incorrectly initially diagnosed as a cardiac myxoma. To accurately diagnose this abnormal mass, we performed the visualization of the heart using different methods - ultrasound (TTE and TEE), X-ray (CT), magnetic resonance (MRI), as well as electrocardiography (ECG) screening for heart rhythm abnormalities. Such a proceeding is novel and ensures high quality of diagnosis as well an appropriate treatment. All visualization methods pointed to LHIS due to its unique features like “dumbbell” shape and lipidous characteristics of this abnormal tissue.
One of the earliest documented instances of LHIS can be traced back to a pathology examination conducted post-mortem, as reported by Prior in 1964 [4], which underscores the importance of autopsy studies in uncovering rare cardiological anomalies. LHIS is primarily composed of hypertrophied and mature multivacuolated adipocytes, which are specialized fat cells that have undergone significant enlargement and alteration, and alongside these, various other cellular components such as fetal fat, enlarged myocytes, myocardial fibers, and differing degrees of fibrotic tissue may also be present, as elucidated in the findings by Burke et al [5] and Gay et al [6], indicating a complex histopathological landscape.
The rarity of occurrence in patients makes the clinical differential diagnosis of cardiac tumors difficult for the treating physician, especially when there is a need to differentiate between a benign and malignant one. Most of the tumors in the heart are benign (80%) as assessed by Reynen [7]. Besides the true neoplasm in the heart, there are also five types of pseudo neoplasm: inflammatory myofibroblastic tumor, hamartoma of mature cardiac myocytes, mesothelial monocytic incidental cardiac excrescences, calcified amorphous tumor, and LHIS [8]. The term LHIS is slightly misleading because histologically the lesion is caused by the proliferation of the fat cells rather than hypertrophy of the fat cells [9]. LHIS can also be differentiated from the lipomas by absence of a capsule [10]. Recognizing a proper type of tumor in the case of LHIS is important to avoid misdiagnosis, which may lead to unnecessary cardiac surgery or give suboptimal treatment. The implementation of advanced diagnostic tools significantly enhances the accuracy of diagnosis, allowing for better differentiation between lipomatous hypertrophy and other cardiac masses and pseudomasses. Recently, there are new approaches also in the Echo diagnostics of right heart masses. Implementation of pulse wave tissue Doppler imaging (PW-TDI) modality may be useful in determining the heart mass characteristics. In TDI, LHIS present a concordant motion with the wall of the right atrium, in synchrony with the phases of the cardiac cycle [11]. But still LHIS diagnostics may be difficult like the differentiation between LHIS and metastatic tumors in PET (due to increased fludeoxyglucose (FDG) uptake on PET, which can be related to the presence of brown fat) [12] or even endocarditis [13]. Propranolol premedication, along with an extended fasting protocol, can help differentiate between LHIS and neoplastic lesions in PET by suppressing brown adipose tissue activity and reducing 18F-FDG uptake, aiding in the accurate characterization of the lesion [14].
LHIS mostly can be treated conservatively; in case of extensive proliferation and obstruction of the vena cava, superior or inferior cardiac surgery may be necessary [15]. Also, the presence of LHIS and the morphological changes in the IAS is prone to abnormal electrical activity within the atrium due to interference with the conduction system connecting the sinoatrial and atrioventricular nodes. This leads to conduction disturbances, atrial fibrillation [16], and even complete heart block [17]. Because of its structure and location, LHIS may cause substantial difficulties during intracardiac procedures. However, in case of a patent foramen ovale (PFO), device closure is typically still possible without necessarily any technical adaptation of the procedure, but the bigger occluder (PFO 35 mm) might be required [18]. If LHIS leads to challenges during transseptal puncture due to its impact on catheter maneuverability and device placement, intracardiac Echo guidance by the puncture may be useful to overcome this difficulty [19].
Conclusion
In summary, the diagnosis of LHIS, as in the case of our patient, may be difficult because it is uncommon in CT, MRI, and Echo and may require the use of more than one visualization modality. The characteristic dumbbell shape is the most apparent sign of LHIS; additionally, the lipidous characteristic of this cardiac mass in CT, MRI, and PET is helpful for differential diagnosis. The blood flow obstruction changes the generally benign nature to more dangerous; in such a case, the extensive fat deposits need to be removed during cardiac surgery. It is also important to look for the heart rhythm abnormalities that make pacemaker implantation for atrioventricular blocks necessary. Although it is not impossible, the occurrence of LHIS may make certain percutaneous cardiac procedures that require atrial septum puncture difficult, such as ablations of the heart arrhythmias. Furthermore, the elevated metabolism of brown fat cells in PET may indicate a malignancy in the IAS, making the diagnosis of LHIS challenging.
Learning points
LHIS must be considered while diagnosing an abnormal mass in the heart. The “dumbbell” shape of the IAS is the unique feature of LHIS. LHIS is mostly benign; however, blood flow obstruction may require a cardiac surgery. LHIS may be diagnosed using Echo, CT, MRI, and PET. Heart rhythm abnormalities may occur. LHIS can make atrial puncture procedures more difficult but not impossible.
Acknowledgments
The authors extend their gratitude for all the invaluable contributions that significantly enhanced the quality of this paper.
Financial Disclosure
There are no financial disclosures and funding in the context of this article.
Conflict of Interest
Authors declare no conflict of interest.
Informed Consent
The patient’s informed consent was obtained to prepare manuscript.
Author Contributions
Adam Golda contributed to study design and literacy search, and wrote manuscript; Beata Bialkowska-Niepon contributed to literacy search and wrote manuscript; Tadeusz Zebik contributed to study design, provided critical feedback, and helped supervise the project.
Data Availability
The data supporting the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
CT: computed tomography; Echo: echocardiography; FDG: fludeoxyglucose; IAS: interatrial septum; LHIS: lipomatous hypertrophy of interatrial septum; MRI: magnetic resonance imaging; PET: positron emission tomography; PFO: patent foramen ovale; PW-TDI: pulse wave tissue Doppler imaging; TEE: transesophageal echocardiography; TTE: transthoracic echocardiography
| References | ▴Top |
- Heyer CM, Kagel T, Lemburg SP, Bauer TT, Nicolas V.
Lipomatous hypertrophy of the interatrial septum: a prospective study of incidence, imaging
findings, and clinical symptoms. Chest. 2003;124(6):2068-2073.
doi pubmed - Beau P, Michel P, Coisne D, Morichau-Beauchant M. Lipomatous
hypertrophy of the cardiac interatrial septum: an unusual complication in long-term home
parenteral nutrition in adult patients. JPEN J Parenter Enteral Nutr.
1991;15(6):659-662.
doi pubmed - Isner JM, Swan CS, 2nd, Mikus JP, Carter BL. Lipomatous
hypertrophy of the interatrial septum: in vivo diagnosis. Circulation.
1982;66(2):470-473.
doi pubmed - Prior JT. Lipomatous hypertrophy of cardiac interatrial
septum. A lesion resembling hibernoma, lipoblastomatosis and infiltrating lipoma. Arch Pathol.
1964;78:11-15.
pubmed - Burke AP, Litovsky S, Virmani R. Lipomatous hypertrophy of
the atrial septum presenting as a right atrial mass. Am J Surg Pathol.
1996;20(6):678-685.
doi pubmed - Gay JD, Guileyardo JM, Townsend-Parchman JK, Ross K.
Clinical and morphologic features of lipomatous hypertrophy (“massive fatty
deposits”) of the interatrial septum. Am J Forensic Med Pathol.
1996;17(1):43-48.
doi pubmed - Reynen K. Frequency of primary tumors of the heart.
Am J Cardiol. 1996;77(1):107.
doi pubmed - Miller DV, Tazelaar HD. Cardiovascular pseudoneoplasms. Arch
Pathol Lab Med. 2010;134(3):362-368.
doi pubmed - O’Connor S, Recavarren R, Nichols LC, Parwani AV.
Lipomatous hypertrophy of the interatrial septum: an overview. Arch Pathol Lab Med.
2006;130(3):397-399.
doi pubmed - Alpert L, Antic T. Lipomatous hypertrophy of the interatrial
septum. Int J Surg Pathol. 2017;25(7):611-612.
doi pubmed - Sonaglioni A, Nicolosi GL, Muti-Schunemann GEU, Lombardo M,
Muti P. Could pulsed wave tissue Doppler imaging solve the diagnostic dilemma of right atrial
masses and pseudomasses? A case series and literature review. J Clin Med.
2024;14(1):86.
doi pubmed pmc - Fan CM, Fischman AJ, Kwek BH, Abbara S, Aquino SL.
Lipomatous hypertrophy of the interatrial septum: increased uptake on FDG PET. AJR
Am J Roentgenol. 2005;184(1):339-342.
doi pubmed - Chiocchi M, Luciano A, De Stasio V, Pugliese L, Di Donna C,
Cerocchi M, Mecchia D, et al. Lipomatous hypertrophy of the interatrial septum: a potential
pitfall resolved on comparing previous PET/CT. Radiol Case Rep. 2023;18(1):222-225.
doi pubmed pmc - Callaud A, Metrard G, Besse H, Bailly M, Thibault F.
Extinction of lipomatous hypertrophy of the interatrial septum FDG uptake with propranolol
premedication. Clin Nucl Med. 2023;48(6):536-537.
doi pubmed pmc - Sef D, Turina MI. Septectomy and biatrial resection for
extensive septal lipomatosis. J Card Surg. 2016;31(11):683-685.
doi pubmed - Erhardt LR. Abnormal atrial activity in lipomatous
hypertrophy of the interatrial septum. Am Heart J. 1974;87(5):571-576.
doi pubmed - Yavar Z, Gilge JL, Patel PJ, Patel AC, Garcia-Cortes RS,
Fetters JK, Fouts AM, et al. Lipomatous hypertrophy of the interatrial septum manifesting as
third degree atrioventricular block. JACC Case Rep. 2020;2(14):2235-2239.
doi pubmed pmc - Meier B. Every patent foramen ovale should be closed.
J Clin Med. 2024;13(11):3355.
doi pubmed pmc - Krafft H, Bahlke F, Popa MA, Deisenhofer I. Catheter
ablation for persistent atrial fibrillation in a patient with extensive lipomatous hypertrophy
of the atrial septum: 3D electroanatomic mapping for ideal procedure planning and performance in
abnormal atrial anatomy. Heart Rhythm O2. 2023;4(11):738-740.
doi pubmed pmc
This
article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0
International License, which permits unrestricted non-commercial use, distribution, and
reproduction in any medium, provided the original work is properly cited.
Journal
of Medical Cases is published by Elmer Press Inc.