| Journal of Medical Cases, ISSN 1923-4155 print, 1923-4163 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Med Cases and Elmer Press Inc |
| Journal website https://jmc.elmerpub.com |
Case Report
Volume 16, Number 3, March 2025, pages 95-101
An Unusual and Successful Pregnancy With Multiple Large Uterine Fibroids Delivered by Cesarean Myomectomy
Dina Marlinaa, f , Aditya Utomoa, Artha Falentin
Putri Susilob, Aditiyono Aditiyonoc, Putri Nadhira Adinda
Adriansyahd, Muhammad Alamsyah Azize
aDepartment of Obstetrics and Gynecology, Universitas Padjadjaran, Bandung,
Indonesia
bDivision of Fertility and Endocrinology Reproduction, Department of
Obstetrics and Gynecology, Universitas Padjadjaran, Bandung, Indonesia
cDivision
of Oncology Gynaecology, Department of Obstetrics and Gynecology, Universitas Jenderal
Soedirman, Purwokerto, Indonesia
dFaculty of Medicine, Universitas Padjadjaran,
Bandung, Indonesia
eDivision of Fetomaternal, Department of Obstetrics and
Gynecology, Universitas Padjadjaran, Bandung, Indonesia
fCorresponding Author:
Dina Marlina, Department of Obstetrics and Gynecology, Universitas Padjadjaran, Bandung, West
Java 40161, Indonesia
Manuscript submitted November 4, 2024, accepted February 1, 2025, published online February 18,
2025
Short title: Pregnancy With Uterine Fibroid
doi: https://doi.org/10.14740/jmc5073
| Abstract | ▴Top |
Uterine fibroids, or myomas, are benign tumors affecting about 68.6% of women, with Indonesia’s Hasan Sadikin Hospital reporting a prevalence between 2.4% and 12.46%. In pregnancy, the incidence drops to 0.1% to 10.7%, but fibroids can still lead to complications. This case study highlights the successful management of a complex pregnancy with multiple large uterine fibroids. A 36- to 37-week primigravida presented with a large intramural fibroid (20 × 15 × 10 cm) at the uterine fundus and six smaller fibroids in the anterior corpus. Despite these challenges, the pregnancy progressed without major issues. A cesarean section was performed, delivering a healthy baby weighing 2,815 g and measuring 46 cm. The case demonstrates effective management of a difficult obstetric situation, emphasizing the importance of tailored care and surgical skill in achieving favorable outcomes for both mother and baby.
Keywords: Pregnancy; Multiple uterine fibroid; Cesarean myomectomy Successful management
| Introduction | ▴Top |
Myoma, known as uterine fibroid, is a most common benign tumor. The prevalence was reported to be 1.830 - 3.150 per 100,000 women in 2019. It affects reproductive women at 35 - 49 years [1]. In Indonesia, the prevalence of uterine fibroids varies between 2.4% and 11.7%, with annual reports from Hasan Sadikin Hospital indicating a peak range of 6.43% to 12.46% [2]. Uterine fibroid was found in about 0.1-10.7% of pregnant women [3, 4]. It is elevated in premenopausal women, individuals with obesity, and those with vitamin D deficiency. It has a lower incidence with increasing parity and women with regular menstrual periods. Uterine fibroid is related to infertility, which affects 2-3% of women and pregnancy complications in any trimester [5]. The size and location of the fibroid are key factors for pregnancy outcomes. There are some indications of taking a cesarean section (CS) with myomectomy, such as age > 40 years and multiple myomas located at the posterior or cornual [5]. The question of whether myomectomy should be performed alongside a CS remains unresolved in modern obstetrics. Until recently, cesarean myomectomy was considered a high-risk procedure due to concerns about significant hemorrhage caused by the increased vascularity of the pregnant uterus, which could lead to higher perioperative morbidity. However, advancements in selective devascularization techniques and anesthesia have encouraged many obstetricians to perform myomectomy during cesarean delivery. This approach aims to prevent the need for a separate surgery in the future, reducing associated risks and costs [6]. This case is one of the examples of a successful pregnancy with multiple uterine fibroids who underwent cesarean myomectomy.
| Case Report | ▴Top |
The patient came for scheduled CS in Obstetric Polyclinic of Hasan Sadikin Hospital with diagnosis of G1P0A0 36 - 37 weeks of pregnancy, intramural uterine fibroid (LO-4 fundal), post conservative management (RSHS, August 18 - 21, 2023), transverse lie. At first, she came due to painless vaginal bleeding of this pregnancy. Thus, she started to take progesterone and should take ultrasonography examinations routinely. She got menarche at 13 years old with a regular cycle. She had no abnormal uterine bleeding or enlargement mass before this pregnancy. She never had taken any contraception and took any medication regularly. Upon physical examination, the vital signs were within normal limits. For anthropometry status, she had 9 kg of additional weight during pregnancy. She was overweight with a body mass index (BMI) of 27.08 kg/m2.
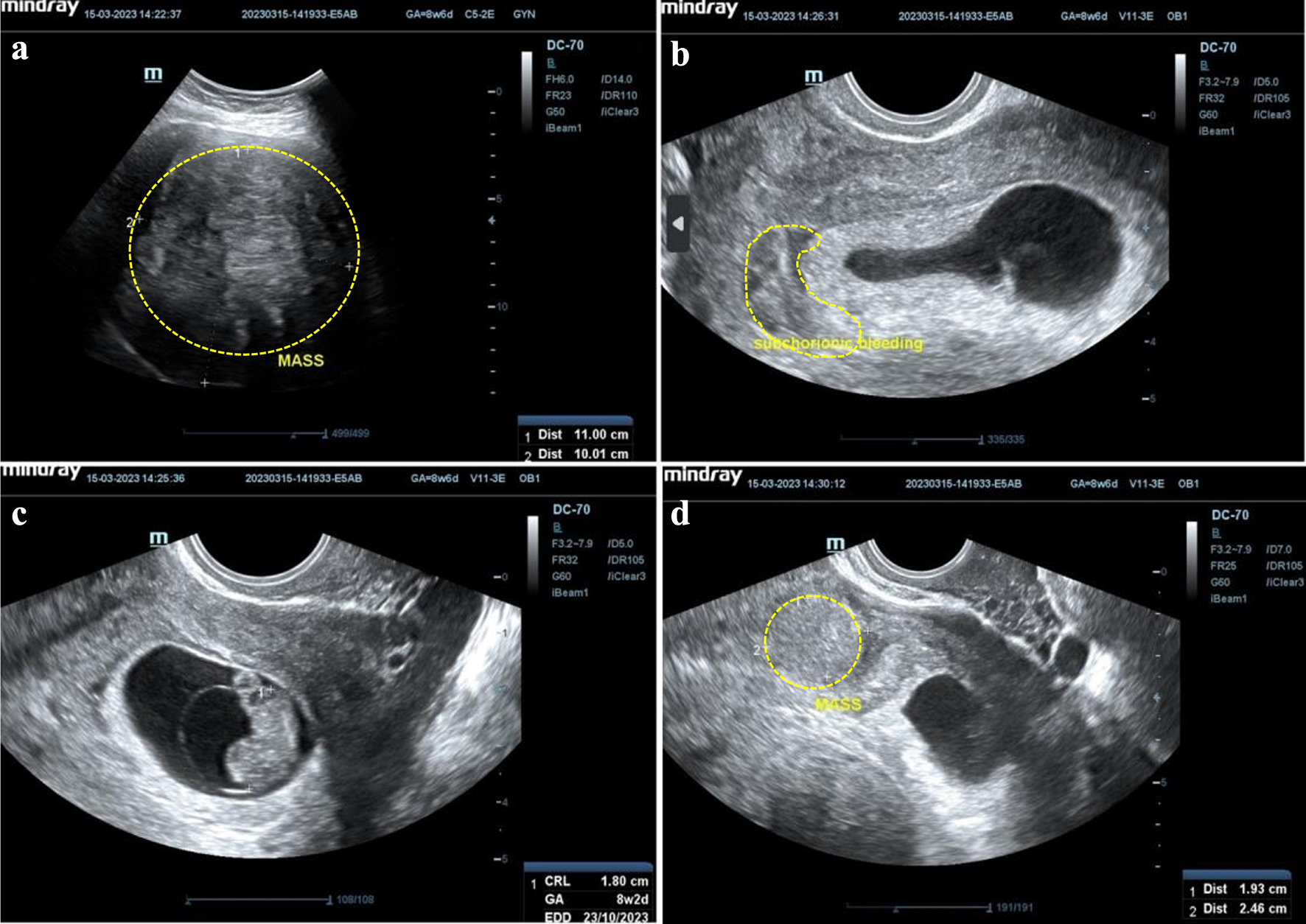
On March 15, 2022, the first ultrasonography examination results showed a single live fetus intrauterine, with a crown-rump length of 1.8 cm according to 8 weeks 2 days of pregnancy, positive fetal heart rate, and positive subchorionic bleeding. The first mass was seen, with hyperechoic density at fundal, measuring 11 × 10 cm. The second mass was seen, with hyperechoic density at the isthmus, measuring 5.46 × 6.27 cm (Fig. 1). She was then advised to control every 2 weeks routinely.
 Click for large image |
Figure 1. Initial ultrasonography examination. (a) A mass, at fundal uterine, hyperechoic density, measuring 11 × 10 cm. (b) Subchorionic bleeding. (c) Single, live fetus, intrauterine, crown-rump length (CRL) 1.8 cm according to 8 weeks and 2 days of pregnancy, positive fetal heart movement. (d) A mass, at isthmus site, hyperechoic density, measuring 5.46 × 6.27 cm. |
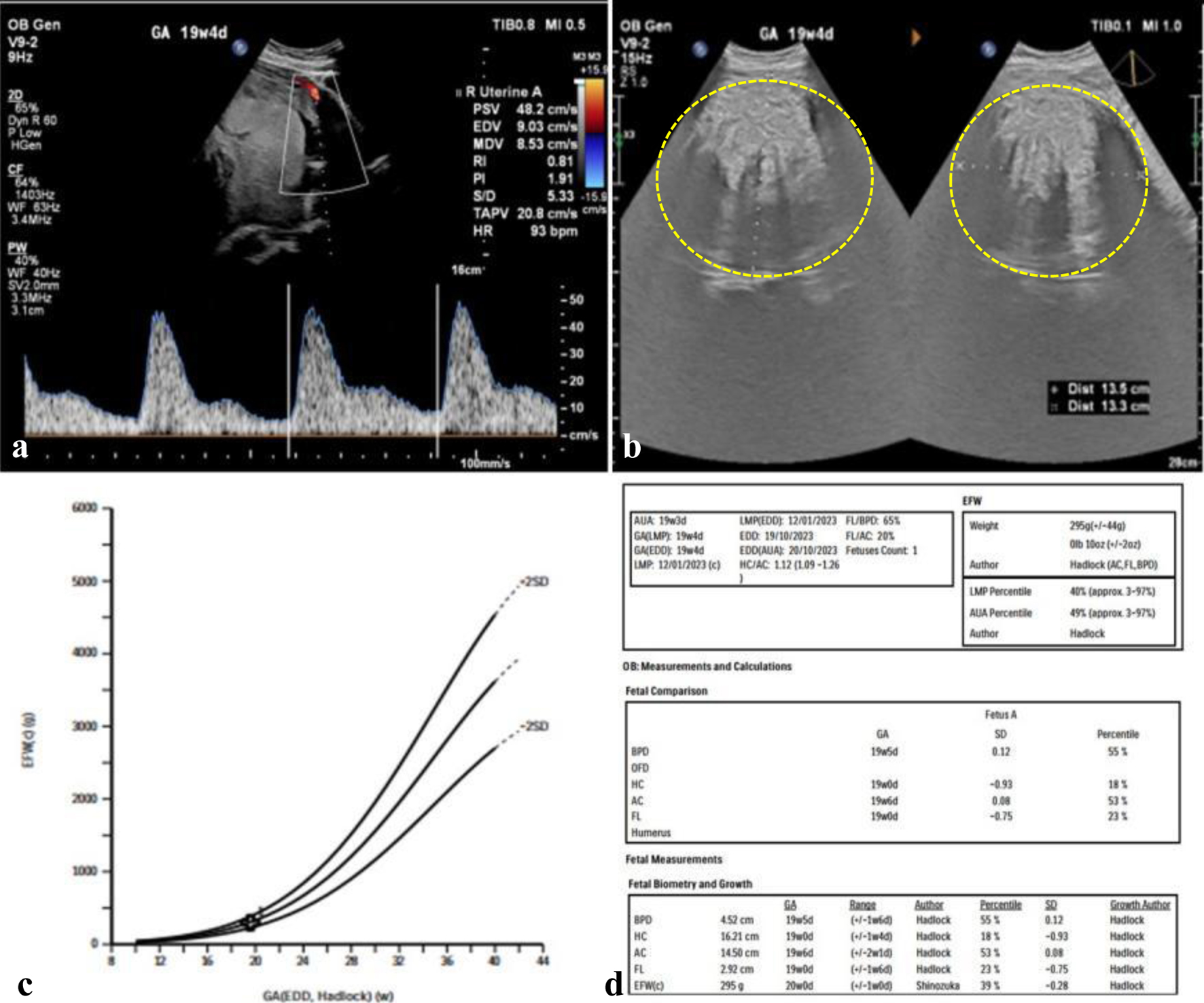
Because the first ultrasonography examination results showed a notching at early pregnancy, she asked to do a fetomaternal ultrasonography examination with the results showing a single live fetus intrauterine, mobile, biometric according to 19 - 20 weeks of pregnancy, with an estimated fetal weight of 295 g, and positive fetal heart rate. Placenta insertion at the fundal extended into the posterior corpus. The uterine fibroid was seen at the posterior corpus, measuring 13 cm (Fig. 2). On velocimetry Doppler examination, it was shown that right uterine artery pulsatility index (PI), resistance index (RI), and systolic/diastolic (S/D) ratio were 1.91, 0.81, and 5.34, respectively, with positive notching. Therefore, she was advised to take aspirin at 19 weeks of pregnancy until a week before elective surgery.
 Click for large image |
Figure 2. Initial fetomaternal ultrasonography examination. (a) Right uterine artery pulsatility index (PI), resistance index (RI), and systolic/diastolic (S/D) ratio of 1.91, 0.81, and 5.34, negative notching. (b) A mass, at posterior corpus, hyperechoic density, measuring 13 × 13 cm. (c, d) Lubchenco curve, gestational age (GA) and estimated fetal weight (EFW) show normal growth lines. |
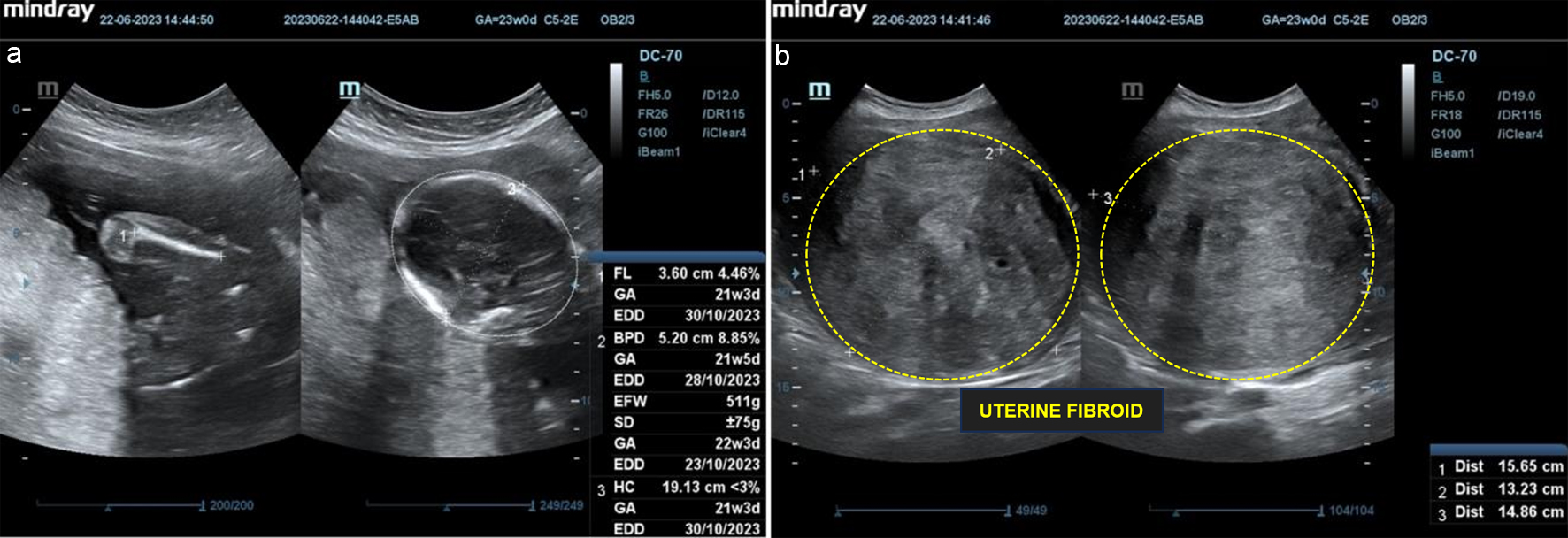
Then, on June 22, 2023, she underwent a next ultrasonography examination at Hasan Sadikin Hospital with the results showing a single live fetus intrauterine, transverse lie, biometric according to 21 - 22 weeks of pregnancy, with an estimated fetal weight of 511 g, and positive fetal heart rate. The ultrasonography revealed a hyperechoic mass with a clear margin line located at the posterior corpus, measuring 15.65 × 13.23 × 14.86 cm, and no neovascularization (Fig. 3).
 Click for large image |
Figure 3. Follow-up ultrasonography examination on second trimester. (a) Single, live fetus, intrauterine, biometric according to 21 - 22 weeks of pregnancy, estimated fetal weight (EFW) 511 g, positive fetal heart rate. (b) A mass, at posterior corpus, hyperechoic density, measuring 15.65 × 13.23 × 14.86 cm, negative neovascularization. |
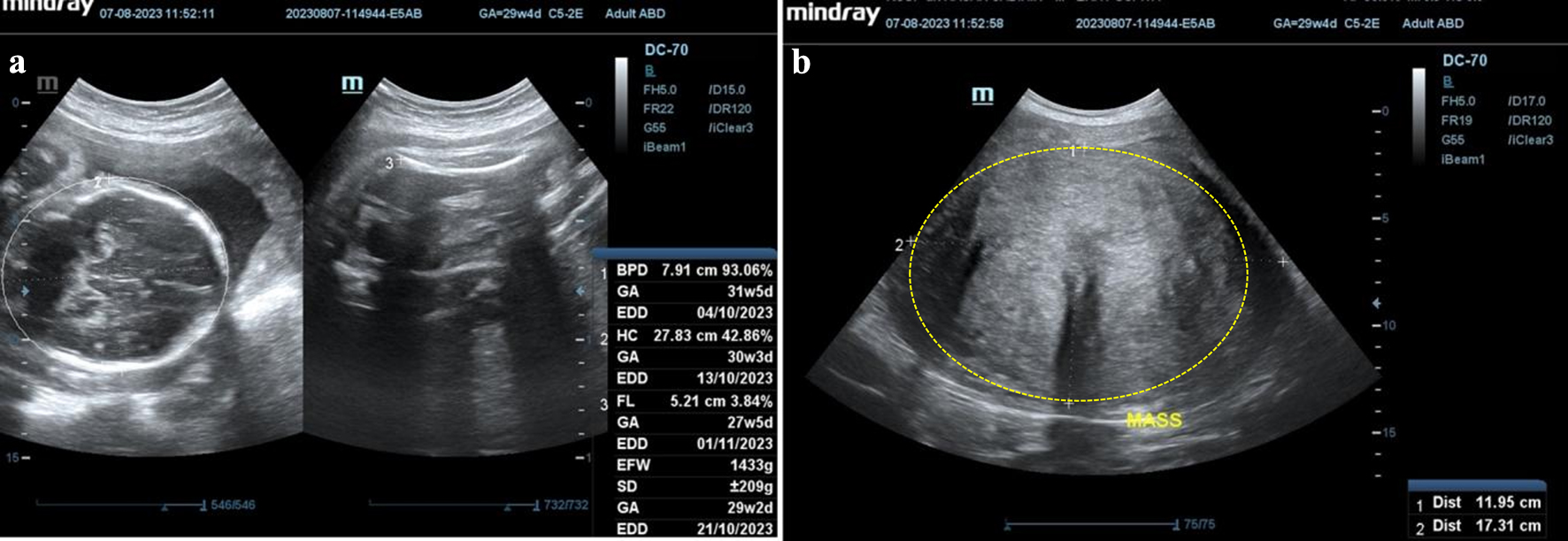
Subsequently, on August 7, 2023, she underwent a follow-up ultrasound examination at Hasan Sadikin Hospital with the results showing a single live fetus intrauterine, transverse lie, biometric according to 30 - 31 weeks of pregnancy, with an estimated fetal weight of 1,433 g, and positive fetal heart rate. A hyperechoic mass was seen, with visible margin line at posterior corpus, measuring 11.95 × 17.31 × 14.86 cm, and negative neovascularization (Fig. 4).
 Click for large image |
Figure 4. Follow-up ultrasonography examination on third trimester. (a) Single fetus, live, intrauterine, biometric according to 30 - 31 weeks of pregnancy, estimated fetal weight (EFW) 1,433 g, positive fetal heart rate. (b) A mass, at posterior corpus, hyperechoic density, measuring 11.95 × 17.31 × 14.86 cm, negative neovascularization. |
She underwent a fourth fetomaternal ultrasonography examination at Hasan Sadikin Hospital with the results showing a single live fetus intrauterine, transverse lie, biometric according to 34 - 35 weeks of pregnancy, with an estimated fetal weight of 2,467 g, trans-cerebellum diameter equal to 36 - 37 weeks of pregnancy, and positive fetal heart rate. A hyperechoic mass was seen, with visible margin line at the posterior corpus, measuring 11.82 × 15.63 × 14.48 cm, and negative neovascularization. In velocimetry Doppler, umbilical PI and S/D ratio were 1.04 and 3.04, respectively, middle cerebral artery (MCA) PI and S/D ratio were 1.72 and 4.88, respectively, right uterine artery S/D ratio was 0.72, and left uterine artery S/D ratio was 0.82.
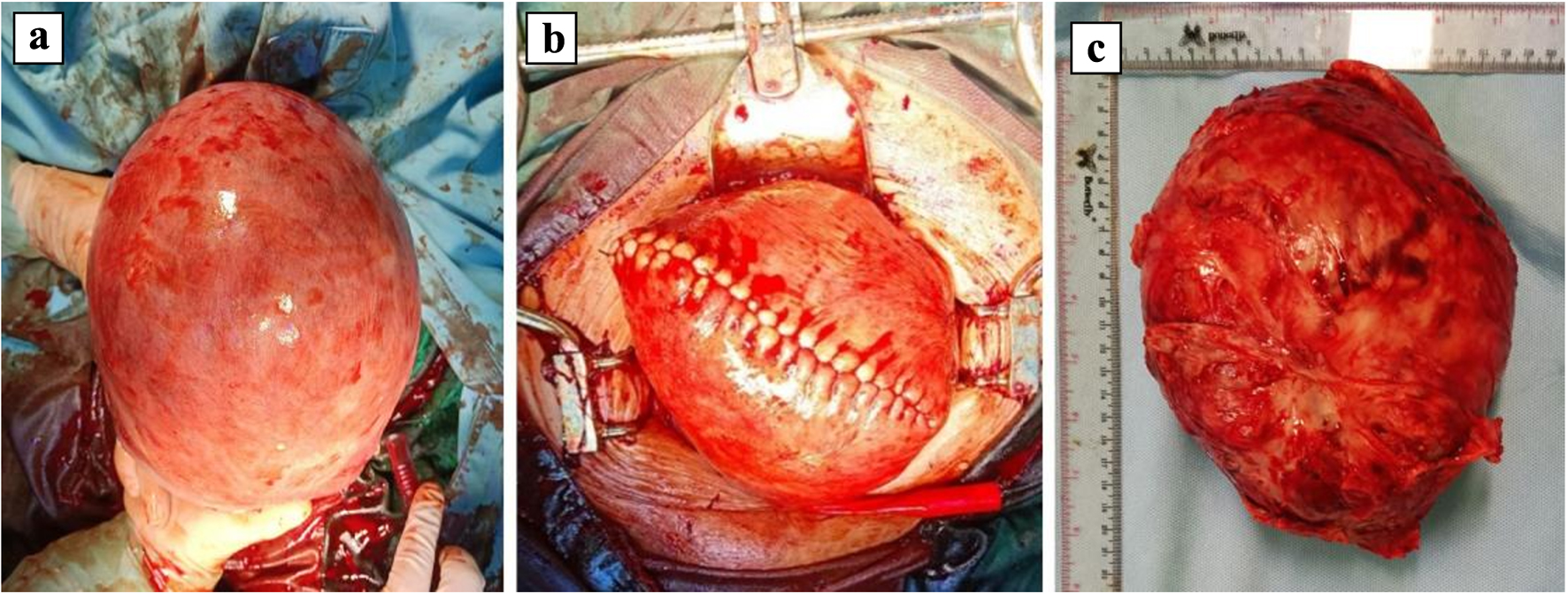
On September 22, 2023, the patient underwent a cesarean myomectomy. The male baby was born with a birth weight of 2,815 g and a fetal length of 46 cm. During exploration, masses from two sides of the uterine corpus were found. A 20 × 15 × 10 cm uterine fibroid intramural mass (LO-4) was located at the uterine fundus and extended to the posterior uterine corpus. Over six solid masses located in the front of the uterine body were identified. The sizes ranged from 0.5 × 0.5 × 0.5 cm to 2.0 × 1.0 × 1.0 cm (LO-5). Both the right and left adnexa were normal (Fig. 5). The patient underwent myomectomy simultaneously. The total amount of blood was 850 cm3.
 Click for large image |
Figure 5. Intraoperative findings showing a large uterine fibroid mass. (a) The uterine view after delivery, inferior view, a mass at fundal, measuring around 20 × 15 × 10 cm. (b) The uterine view after enucleation and reparation, superior view. (c) The specimen mass after enucleation procedure. |
Upon examination of pathological anatomical findings, the macroscopic results showed: 1) a tissue tumor measuring 15 × 12 × 10 cm, with a brownish-white color, soft texture, and a white solid mass displaying a whorl-like pattern. No necrotic region was observed. 2) A tissue tumor measuring 14 × 11 × 9 cm, with a brownish-white color, soft texture, and a white solid mass with a whorl-like structure, and no necrotic area. 3) There were five tissue tumors, varying in size from 1 × 0.7 × 0.4 cm to 0.3 cm. The objects seemed brownish white, velvety, with a white solid bulk displaying a whorl-like pattern. No necrotic regions were detected. The microscopic inspection revealed a solid tumor mass with hyperplasia of myocyte cells, with minimal narrative framework, and typical nucleus cell. Fibrous collagen stromal tissues including inflammatory lymphocytes and plasma cells, as well as vascular dilation and hemorrhaging were observed. No cancer was detected. The patient was admitted to the hospital for a duration of 2 days. No bleeding was observed on the first day following surgery, as confirmed by post-surgical laboratory tests. One week post-surgery, the patient had a follow-up appointment reporting no issues, and the ultrasonography results were favorable.
| Discussion | ▴Top |
Uterine fibroids are observed in approximately 0.1-10.7% of pregnancies [4]. These fibroids are influenced by various risk factors, including premenopausal age, nulliparity, obesity, family history, elevated BMI, and vitamin D deficiency, while high parity, later age at first childbirth, and regular menstrual cycles appear to have protective effects [1, 4]. In this case, the patient was a 35-year-old nullipara with an overweight BMI of 27.08 kg/m2 prior to pregnancy.
Symptoms of uterine fibroids during pregnancy can include abnormal uterine bleeding, pain, and urinary or gastrointestinal disturbances, although many fibroids remain asymptomatic. In the present case, the patient exhibited symptoms during early pregnancy that improved in subsequent trimesters despite the presence of a large fibroid [7].
On ultrasound, uterine fibroids are typically described as solid, round, well-circumscribed, hypoechoic, and heterogeneous lesions located within the myometrium. They often exhibit acoustic shadowing along their edges and may display internal fan-shaped shadowing. On color Doppler imaging, circumferential blood flow around the lesion is frequently observed [8]. The echogenicity variations are determined by the extent of calcification and amount of fibrous tissue. The accuracy of ultrasound in identifying fibroids during pregnancy is limited to 1.4-2.7% because of challenges in distinguishing between normal uterine and myometrial thickness [5]. In this case, during an ultrasound examination at 8 weeks of pregnancy, the patient was found to have a uterine fibroid measuring 11 × 10 cm. By 20 weeks of pregnancy, at the Fetal-Maternal Polyclinic, the fibroid had grown to 11.82 × 15.63 × 14.48 cm. Additionally, two smaller uterine fibroids were identified during surgery, which had previously gone undetected due to their minimal size.
The growth of uterine fibroids during pregnancy is influenced by hormonal changes, particularly increased levels of estrogen and progesterone, which contribute to their enlargement, particularly during the first and second trimesters [9]. Fibroids tend to stabilize or shrink in the late third trimester, especially in female fetuses, likely due to differences in hormonal and angiogenic factors [10].
Pregnant women with fibroids face an elevated risk of complications throughout pregnancy, including miscarriage, preterm labor, abnormal placental attachment, fetal malpresentation, and postpartum hemorrhage [4, 5]. The likelihood of adverse outcomes is influenced by the size, number, and location of the fibroids. Intramural and submucosal fibroids, in particular, are associated with higher complication rates. Studies report live birth rates ranging from 21.8% to 44.2% depending on fibroid location, with anterior fibroids correlating with lower rates [11]. However, in this case, the patient experienced no significant complications after the first trimester, and the pregnancy was successfully managed until termination at 36 weeks.
In Indonesia, the management of uterine fibroids aligns with national and international practices, emphasizing individualized treatment based on factors such as the patient’s age, symptom severity, desire to preserve fertility, and the size and location of the fibroids [12]. Initial management often involves medical therapies aimed at alleviating symptoms. These may include the use of progestogens, the levonorgestrel-releasing intrauterine device, tranexamic acid, nonsteroidal anti-inflammatory drugs, or gonadotropin-releasing hormone (GnRH) analogs to manage abnormal uterine bleeding [13].
While many fibroids remain asymptomatic during pregnancy, some can lead to complications such as pain, bleeding, or interference with fetal development. Conservative management is often preferred, focusing on monitoring and symptom relief, given the risks associated with surgical interventions during pregnancy. Myomectomy, the surgical removal of fibroids, is generally avoided during pregnancy due to potential complications like significant blood loss and preterm labor [12]. However, in select cases where fibroids cause severe symptoms unresponsive to medical therapy, myomectomy may be considered. It is essential for pregnant women with fibroids to receive regular prenatal care, allowing healthcare providers to monitor fibroid growth and manage any arising complications promptly. Treatment plans should be tailored to the individual’s condition, balancing the benefits and risks to ensure the safety of both mother and child [13]. The decision for cesarean myomectomy in this case was based on the large size and multiple nature of the fibroids, which posed potential risks to the pregnancy and delivery.
Cesarean myomectomy, the concurrent removal of uterine fibroids during a CS, has traditionally been approached with caution due to concerns about significant hemorrhage and postoperative complications [6]. However, recent studies suggest that, in carefully selected patients, this procedure can be performed safely without increasing the risk of adverse outcomes [6, 14].
Several studies suggest that performing a myomectomy during a CS is not as high-risk as traditionally believed. Enucleation is often facilitated by the softened tissues during pregnancy [15-17]. Patients should be counseled about the feasibility of myomectomy, with the final decision depending on factors such as the size, number, and location of the fibroids, and intramural myomectomy should be approached cautiously. Only fibroids that are likely to require future surgical intervention should be removed during CS [6].
Currently, there are no universally accepted guidelines for the indications and contraindications of cesarean myomectomy. Therefore, careful patient counseling and individualized assessment are essential, with safety being the primary consideration. Indications for cesarean myomectomy well described in various literature include symptomatic fibroids causing pain, rapid growth, or those obstructing the birth canal, which could complicate delivery. The decision to proceed with myomectomy during CS should be individualized, taking into account factors such as the size, number, and location of the fibroids, as well as the surgeon’s experience and the availability of resources to manage potential hemorrhage [6]. Studies have demonstrated that with proper patient selection and surgical expertise, cesarean myomectomy does not significantly increase operative time or blood loss compared to CS alone. Therefore, cesarean myomectomy can be considered a viable option for managing fibroids in pregnant patients when specific indications are present [18].
The single-case nature of this report provides an in-depth exploration of a unique clinical scenario, yet we acknowledge its inherent limitation in terms of generalizability. Future studies involving larger cohorts could validate and expand upon our findings, providing more robust evidence on the diagnostic and management protocols for pregnancies complicated by uterine fibroids. These studies could also investigate long-term maternal and neonatal outcomes, assess the efficacy of interventions like routine Doppler surveillance or conservative management with progesterone, and explore variations in fibroid growth and vascularization. Such data would help establish evidence-based guidelines and improve decision-making in similar complex cases.
Conclusion
This patient is presented with vaginal bleeding during the early stage of her pregnancy. She developed a large uterine fibroid throughout the early stages of her pregnancy. Despite the large size of the fibroid, the pregnancy proceeds without complications until termination is scheduled. The patient who underwent myomectomy gave birth to a healthy infant without any complications. This is an exceptional situation as it involves a successful and healthy pregnancy, a healthy newborn despite the presence of several large uterine fibroids, and a safe delivery through cesarean myomectomy without any difficulties.
Acknowledgments
None to declare.
Financial Disclosure
The authors received no financial support for the research, authorship, and/or publication of this article.
Conflict of Interest
The authors reported no conflict of interest.
Informed Consent
Written informed consent was obtained from the patient for publication of the case report and accompanying images.
Author Contributions
All authors contributed to the conceptualization of the presented case report. DM wrote the initial draft of the case report with input from all authors. AU and AFPS made substantial contribution to the design of the case report. All authors drafted or critically revised the case report for important content, approved the version to be published, and agreed to integrity or accuracy of any part of the work. DM and AA provided oversight and leadership responsibility for the case report execution. PNAA and MAA contributed significantly to resources for case report execution.
Data Availability
The authors declare that the data supporting the findings of this study are available within the article.
| References | ▴Top |
- Lou Z, Huang Y, Li S, Luo Z, Li C, Chu K, Zhang T, et al.
Global, regional, and national time trends in incidence, prevalence, years lived with disability
for uterine fibroids, 1990-2019: an age-period-cohort analysis for the global burden of disease
2019 study. BMC Public Health. 2023;23(1):916.
doi pubmed - Ilma N, Tjahyadi D, Judistiani T. The Relationship of Age,
Parity and Body Mass Index as Risk Factors to the Incidence of Uterine Myoma in Dr. Hasan
Sadikin General Hospital. Althea Medical Journal. 2015;2.
doi - Choudhary A, Inamdar SA, Sharma U. Pregnancy with uterine
fibroids: obstetric outcome at a tertiary care hospital of central India. Cureus.
2023;15(2):e35513.
doi pubmed - Tirnovanu MC, Lozneanu L, Tirnovanu SD, Tirnovanu VG,
Onofriescu M, Ungureanu C, Toma BF, et al. Uterine fibroids and pregnancy: a review of the
challenges from a Romanian Tertiary Level Institution. Healthcare (Basel). 2022;10(5).
doi pubmed - Freytag D, Gunther V, Maass N, Alkatout I. Uterine fibroids
and infertility. Diagnostics (Basel). 2021;11(8).
doi pubmed - Kathpalia SK, Arora D, Vasudeva S, Singh S. Myomectomy at
cesarean section: A safe option. Med J Armed Forces India. 2016;72(Suppl
1):S161-S163.
doi pubmed - Wilde S, Scott-Barrett S. Radiological appearances of
uterine fibroids. Indian J Radiol Imaging. 2009;19(3):222-231.
doi pubmed - Palheta MS, Medeiros FDC, Severiano ARG. Reporting of
uterine fibroids on ultrasound examinations: an illustrated report template focused on surgical
planning. Radiol Bras. 2023;56(2):86-94.
doi pubmed - Schock H, Zeleniuch-Jacquotte A, Lundin E, Grankvist K, Lakso
HA, Idahl A, Lehtinen M, et al. Hormone concentrations throughout uncomplicated pregnancies: a
longitudinal study. BMC Pregnancy Childbirth. 2016;16(1):146.
doi pubmed - Delli Carpini G, Verdecchia V, Papiccio M, Grelloni C,
Ciavattini A. Comparison of uterine fibroids' growth pattern during pregnancy according to fetal
sex: an observational study. Biol Sex Differ. 2019;10(1):53.
doi pubmed - Zhang Y, Hua KQ. Patients' age, myoma size, myoma location,
and interval between myomectomy and pregnancy may influence the pregnancy rate and live birth
rate after myomectomy. J Laparoendosc Adv Surg Tech A. 2014;24(2):95-99.
doi pubmed - Harzif AK. Konsensus mioma uteri. Department of Obstetrics and Gynecology Clinic. Available from: https://scholar.ui.ac.id/en/publications/konsensus-mioma-uteri.
- Vitale SG, Padula F, Gulino FA. Management of uterine
fibroids in pregnancy: recent trends. Curr Opin Obstet Gynecol. 2015;27(6):432-437.
doi pubmed - Ghaemmaghami F, Karimi-Zarchi M, Gharebaghian M, Kermani T.
Successful myomectomy during cesarean section: case report & literature review.
Int J Biomed Sci. 2017;13(2):119-121.
pubmed - Bhatla N, Dash BB, Kriplani A, Agarwal N. Myomectomy during
pregnancy: a feasible option. J Obstet Gynaecol Res. 2009;35(1):173-175.
doi pubmed - Gbadebo AA, Charles AA, Austin O. Myomectomy at caesarean
section: descriptive study of clinical outcome in a tropical setting. J Ayub Med Coll
Abbottabad. 2009;21(4):7-9.
pubmed - Hassiakos D, Christopoulos P, Vitoratos N, Xarchoulakou E,
Vaggos G, Papadias K. Myomectomy during cesarean section: a safe procedure?
Ann N Y Acad Sci. 2006;1092:408-413.
doi pubmed - Awoleke JO. Myomectomy during caesarean birth in
fibroid-endemic, low-resource settings. Obstet Gynecol Int. 2013;2013:520834.
doi pubmed
This
article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0
International License, which permits unrestricted non-commercial use, distribution, and
reproduction in any medium, provided the original work is properly cited.
Journal
of Medical Cases is published by Elmer Press Inc.