| Journal of Medical Cases, ISSN 1923-4155 print, 1923-4163 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, J Med Cases and Elmer Press Inc |
| Journal website https://jmc.elmerpub.com |
Case Report
Volume 17, Number 6, June 2026, pages 239-243
The Effect of Laparoscopic Dermoid Cystectomy on Anti-Mullerian Hormone: A Case Series
Praneel Kumara, b, e , Harry Merkura, c, Peter Russelld, Clare Wonga, c
aDepartment of Obstetrics and Gynaecology, Blacktown Hospital, Sydney, Australia
bAdelaide Medical School, Faculty of Health and Medical Sciences, Adelaide University, Adelaide, Australia
cFaculty of Medicine, Western Sydney University, Campbelltown, Australia
dDepartment of Anatomical Pathology, Douglass Hanly Moir Pathology, Macquarie Park, Australia
eCorresponding Author: Praneel Kumar, Adelaide Medical School, Faculty of Health and Medical Sciences, Adelaide University, Adelaide, Australia
Manuscript submitted January 3, 2026, accepted March 17, 2026, published online April 29, 2026
Short title: Dermoid Cystectomy and AMH
doi: https://doi.org/10.14740/jmc5276
| Abstract | ▴Top |
Laparoscopic cystectomy for benign ovarian pathologies overall has been shown to reduce anti-Mullerian hormone (AMH), an important biomarker of ovarian reserve and fertility; however, the effect of dermoid cystectomy on ovarian reserve remains unclear. We sought to measure the change in AMH from before and after planned laparoscopic dermoid cystectomy at our surgical center in a case series. Females of reproductive age between 18 and 40 years presenting with a pre-operative diagnosis of a unilateral dermoid cyst on pelvic ultrasound and an indication for laparoscopic cystectomy were recruited. AMH levels were measured pre-operatively and repeated post-operatively between 6 and 8 weeks and the histology was checked to confirm a dermoid cyst. The laparoscopic surgery was undertaken using a standard technique at our center by senior gynecologists. A non-parametric Wilcoxon signed-rank test was performed to assess the difference between paired serum AMH samples. Of the seven females with dermoid cyst on final histopathology, there was no statistically significant difference observed between the pre-operative and post-operative AMH levels (W-value 13, P-value not less than 0.05). Our case series did not show any difference between pre-operative and post-operative AMH results following laparoscopic dermoid cystectomy and more data are required on the impact on ovarian reserve from future studies.
Keywords: Dermoid cyst; Fertility; Laparoscopy
| Introduction | ▴Top |
Dermoid cysts, also called mature cystic teratomas, are a benign ovarian cyst and account for 70% of ovarian cysts in females aged less than 30 years of age [1]. Dermoid cysts that cause abdominal pain or enlarge are recommended for surgical removal. Laparoscopic cystectomy, where available, is the standard of care given the advantages of minimally invasive surgery such as faster recovery time, reduced post-operative pain, and improved cosmesis [2, 3].
The effect on fertility is an important consideration when performing ovarian surgery on reproductive aged females. Characteristics of the cyst such as endometrioma histology, increased size, and bilaterality have been shown to decrease ovarian reserve following cystectomy [2–8]. Injury to the ovary resulting from cystectomy can also occur and decrease ovarian reserve [4, 9] which can be more pronounced with certain surgical techniques such as the use of electrosurgery for hemostasis [2, 8, 10].
Current studies use a variety of measures to assess the effect of cystectomy on ovarian reserve. Anti-Mullerian hormone (AMH) is released by early-stage follicles in the ovary and levels decrease with increasing age [2, 11]. AMH is a commonly used biomarker given that it is simple to collect with venepuncture and levels remain stable during the menstrual cycle [2]. Studies measure AMH following cystectomy at different time points, ranging from 1 day post-operatively to 12 months [9, 12, 13]. Other assessments of ovarian reserve include follicle stimulating hormone levels, pelvic ultrasound (for ovarian volume, Doppler, and antral follicle counts), histopathology specimens for follicle counts, and in-vitro fertilization (IVF) cycle success rates [1, 4, 5, 12, 14].
The current evidence on the effect of dermoid cystectomy on ovarian reserve is lacking. A meta-analysis of the excision of non-endometriotic benign cysts, which included dermoid cysts, showed that cystectomy decreased serum AMH levels by a mean of 1.14 ng/mL (95% confidence interval (CI) −1.36, −0.92) (equivalent to 8.1 pmol/L) over 1 to 6 months [11]. However, by combining all benign cysts in a single group, the effect of dermoid cystectomy on ovarian reserve cannot be distinguished. Primary studies also group dermoid cystectomies with other benign pathology and dermoid cysts are often in the minority within the benign pathology grouping [5, 6, 12, 14–16]. The handful of studies that separately report the effect of dermoid cystectomy on ovarian reserve have relatively small sample sizes (ranging from 7 to 33) [7–9, 17, 18]. These studies also show conflicting results. For example, Lind et al reported a 25% reduction in AMH levels 6 months following dermoid cystectomy [17], whereas Henes et al did not detect a change from pre- to post-operative AMH levels [7]. Amooee et al reported that declines in AMH levels were greatest with dermoid cysts compared to mucinous cystadenomas and serous cystadenomas [18].
The effect of dermoid cystectomy on ovarian reserve merits further investigation as they are distinct from other benign ovarian cysts. Dermoid cysts contain inflammatory material and spillage of the cyst contents during surgery can result in chemical peritonitis, which may affect ovarian function [1]. Dermoid cysts are also relatively common and information relating to the effect of dermoid cystectomy on fertility can aid in the counseling of patients planned for surgery [1]. To understand the effect of planned laparoscopic dermoid cystectomy on ovarian reserve, we measured the change in serum AMH before and after surgery in a small case series. Our secondary aim was to record any ovarian follicles observed on the histopathology specimen after excision of the dermoid cyst.
| Case Report | ▴Top |
Methods
Study design
We performed a study where participants acted as their own controls given the pre-test post-test design. Our study was concerned with measuring changes in AMH levels within a participant as opposed to between participants. Clinical differences between participants are presented for completeness in the case series.
Study participants
Females aged 18–40 years, referred to the gynecology clinic with a suspected dermoid cyst on pelvic ultrasound and requiring laparoscopic ovarian cystectomy, were eligible. Indications for surgery included symptoms due to the ovarian cyst, such as pelvic pain, and persistence or enlargement of the ovarian cyst. Exclusion criteria included suspicion of malignancy or previous malignancy, non-dermoid cyst on pelvic ultrasound and/or final histopathology, previous diagnosis of infertility of any cause, changes in hormonal medication use that could affect AMH measurements from participant enrollment to their post-operative AMH measurement, pituitary, thyroid or adrenal disorders and pregnancy. No participants had taken oral contraceptive pills within 3 months of the study enrollment or the AMH measurements.
Surgical procedure
Specialist gynecologists with training in minimally invasive surgery at the same center performed the operations. All participants were consented for a unilateral laparoscopic ovarian cystectomy. Following general anesthesia, an umbilical incision was made for abdominal entry, pneumoperitoneum was established, and a 10 mm umbilical trocar inserted. Two accessory trocars were placed under direct laparoscopic vision in the lower abdominal quadrant. Using monopolar scissors, the ovarian cyst was incised, the capsule identified, and the cyst removed using traction with laparoscopic forceps, taking care to preserve the ovarian parenchyma and avoiding spillage of the cyst contents. Hemostasis was achieved with sutures, diathermy, or sealants. Conversion to laparotomy was performed in an emergency or if the cyst could not be removed laparoscopically. Following surgery, the participants were observed for a maximum of 48 h and then discharged.
Outcome measurement
Venepuncture was used to collect a pre-operative (baseline) and post-operative serum AMH sample, regardless of the menstrual cycle day. The pre-operative serum AMH was collected within 4 months of surgery from all participants. The post-operative sample was collected between 6 and 8 weeks following surgery from all participants. This timeframe allowed for inflammation to have resolved post-surgery. The samples for each participant were tested using the same immunoassay method at the central laboratory, which had a lower limit of quantitation of 1 pmol/L and an inter-assay coefficient of variation of less than 5.6%. The excised ovarian cyst was reviewed on histopathology to confirm a dermoid cyst, and the presence of any primordial follicles observed by a qualified pathologist in the histopathology report was recorded. The presence of primordial follicles was not a quantitative assessment.
Statistical analysis
The paired pre-operative and post-operative serum AMH concentrations for each participant were compared using a non-parametric, two-tailed, Wilcoxon’s signed-rank test. The test is appropriate for dependent samples and small sample sizes. A P-value less than 0.05 was considered statistically significant. Statistical analysis was performed using Stata (StataCorp, Texas, USA, version 18.5).
Ethical approval
All participants provided written informed consent prior to enrollment. The study was approved by the Western Sydney Local Health District Human Research Ethics Committee (approval number 2020/ETH02973) and followed all ethical guidelines.
Results
We recruited 10 participants for our study; however, two were excluded from the final analysis as they had a non-dermoid cyst on final histopathology and one participant did not complete their post-operative AMH measurement.
The seven participants in our case series had an age range from 18 to 40 years with a unilateral dermoid cyst, varying in size from 4 to 8 cm (see Table 1 for case information). Five participants were nulliparous.
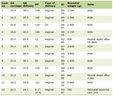 Click to view | Table 1. Participant Case Details |
The main indication for surgery was pelvic pain (n = 5/7). Four participants had spillage of the dermoid cyst intra-operatively. One laparoscopic surgery was converted to open surgery due to difficulty removing the dermoid cyst while avoiding spillage. Diathermy for hemostasis was used in only one participant. There were no post-operative complications noted.
There was no statistically significant difference between the pre-operative AMH and post-operative AMH values (Wilcoxon’s signed-rank test P-value 0.9375). Three participants had histopathology samples noting the presence of primordial follicles.
| Discussion | ▴Top |
Our case series did not find a statistically significant difference in females of reproductive age planned for laparoscopic dermoid cystectomy in pre- to post-operative serum AMH levels. This is a similar finding to Henes et al study (n = 7) [7] that did not detect a difference in AMH levels following dermoid cystectomy, however, differs from several other studies, including a systematic review of all benign non-endometriotic ovarian cysts (n = 367) and dermoid cysts (n = 23), respectively [11, 18]. Histopathology reports noted the presence of primordial follicles in only three out of the seven participants.
Inferring the impact of dermoid cystectomies on ovarian reserve is currently required given the paucity of studies investigating this effect directly. Evidence from a clinical trial which compared different methods of hemostasis during dermoid cystectomy can be informative [13]. Liang et al (n = 80) reported a statistically significant decrease, ranging from 16% to 20% in serum AMH levels at 12 months after endoscopic dermoid cystectomy compared with pre-operative levels, irrespective of the hemostasis method used [13]. This would suggest that dermoid cystectomy reduces ovarian reserve similar to other benign ovarian cystectomies. Huang et al study (n = 71) which investigated single-port versus conventional laparoscopy for dermoid cystectomy reported a 15% decrease from pre-operative to post-operative AMH levels at 4 weeks in both arms [19].
When a decrease in serum AMH has been detected post-operatively, several studies have found recovery. Ding et al (n = 90) reported that while serum AMH levels decreased following laparoscopic cystectomy for benign ovarian cysts at 1 month, there was no difference at 6 and 12 months when compared to pre-operative levels [12]. Similar findings have also been replicated by Li et al (n = 56) [20] at 6 months. Chang et al (n = 20) [5] and Amooee et al (n = 23) [18] reported AMH recovery as soon as 3 months post-cystectomy. While the recovery of AMH levels is not a universal finding in the current literature [13], these results can provide some reassurance on the effect of fertility during patient counseling. Similarly, serum FSH levels following benign non-endometriotic cystectomies have also been reported to remain stable from baseline to 6 months post-operatively [4, 12, 20].
Strengths of our study include its prospective design, adherence to standardized operative technique, and measurement of AMH levels using the same assay method for each participant. Our study also provides data specific for dermoid cysts, which are not consistently reported in the current literature. It can therefore inform future systematic reviews and meta-analysis on this topic.
While our case series cannot provide definitive evidence on the effect of laparoscopic dermoid cystectomy on ovarian reserve due to the small sample size, it can inform future studies. For example, we only measured one marker of ovarian reserve post-operatively at one point in time, and changes in AMH levels may also not indicate changes in fertility levels, therefore additional markers could be considered in future studies. Moreover, there is significant variation in the timing of AMH measurement post-surgery in the literautre [9]; studies showing recovery of AMH at different time intervals [12]; and no agreed threshold at which a particular level of AMH decline is deemed clinically significant. Consensus on the types of ovarian reserve markers, frequency of measurement, and the degree of change within these markers that are clinically significant is needed. Future studies that control for different types of ovarian cysts (such as size, number), surgical techniques, and patient factors (such as age) are also required. Participant age is also an important determinant of AMH levels. Two of the participants in our case series were over 35 years of age and they had the lowest AMH levels at baseline. The impact of ovarian cystectomy in participants greater than 35 years therefore needs particular consideration in pre-operative counseling.
Learning points
Ovarian cystectomy can result in ovarian injury and a decrease in ovarian reserve, which can be more pronounced with the use of electrosurgery for hemostasis.
The current literature suggests that there is a reduction in ovarian reserve following benign ovarian cystectomies overall, and this may recover within 1 year of surgery.
Individualized patient counseling, which takes into account their age, the cyst size, type, and number, should be considered pre-operatively.
Conclusion
Our case series did not find a statistically significant change in AMH levels pre-operative to post-operative following laparoscopic dermoid cystectomy. The effect on fertility following dermoid cystectomies needs to be considered during counseling with patients and more data are required from future studies.
Acknowledgments
None to declare.
Financial Disclosure
This study was not supported by any sponsor or funder.
Conflict of Interest
The authors have no conflict of interest to declare.
Informed Consent
Participants have given their written informed consent and the study protocol has been approved by the Western Sydney Local Health District Human Research Ethics Committee, approval number (2020/ETH02973).
Author Contributions
Praneel Kumar: data curation, formal analysis, investigation, writing – original draft, review & editing. Harry Merkur: project administration, conceptualization, methodology, supervision, writing – review & editing. Peter Russell: methodology, investigation, writing – review & editing. Clare Wong: project administration, methodology, supervision, writing – review & editing.
Data Availability
The authors declare that data supporting the findings of this study are available within the article.
Abbreviations
AMH: anti-Mullerian hormone; IVF: in-vitro fertilization
| References | ▴Top |
- Legendre G, Catala L, Moriniere C, Lacoeuille C, Boussion F, Sentilhes L, Descamps P. Relationship between ovarian cysts and infertility: what surgery and when? Fertil Steril. 2014;101(3):608-614.
doi pubmed - Kalampokas T, Kamath MS, Kalampokas E. AMH after laparoscopic surgery of the ovaries: a review. Gynecol Endocrinol. 2013;29(5):408-411.
doi pubmed - Alammari R, Lightfoot M, Hur HC. Impact of cystectomy on ovarian reserve: review of the literature. J Minim Invasive Gynecol. 2017;24(2):247-257.
doi pubmed - Bareghamyan H, Chopikyan A, Petrosyan M, Shahverdyan N, Harutyunyan A. Influence of ovarian cysts on ovarian reserve and fertility: a case-control study. Int J Gynaecol Obstet. 2024;165(2):424-430.
doi pubmed - Chang HJ, Han SH, Lee JR, Jee BC, Lee BI, Suh CS, Kim SH. Impact of laparoscopic cystectomy on ovarian reserve: serial changes of serum anti-Mullerian hormone levels. Fertil Steril. 2010;94(1):343-349.
doi pubmed - Chen Y, Pei H, Chang Y, Chen M, Wang H, Xie H, Yao S. The impact of endometrioma and laparoscopic cystectomy on ovarian reserve and the exploration of related factors assessed by serum anti-Mullerian hormone: a prospective cohort study. J Ovarian Res. 2014;7:108.
doi pubmed - Henes M, Engler T, Taran FA, Brucker S, Rall K, Janz B, Lawrenz B. Ovarian cyst removal influences ovarian reserve dependent on histology, size and type of operation. Womens Health (Lond). 2018;14:1745506518778992.
doi pubmed - Mansouri G, Safinataj M, Shahesmaeili A, Allahqoli L, Salehiniya H, Alkatout I. Effect of laparoscopic cystectomy on ovarian reserve in patients with ovarian cyst. Front Endocrinol (Lausanne). 2022;13:964229.
doi pubmed - Chun S, Cho HJ, Ji YI. Comparison of early postoperative decline of serum antiMullerian hormone levels after unilateral laparoscopic ovarian cystectomy between patients categorized according to histologic diagnosis. Taiwan J Obstet Gynecol. 2016;55(5):641-645.
doi pubmed - Lin YH, Hsia LH, Huang YY, Chang HJ, Lee TH. Potential damage to ovarian reserve from laparoscopic electrocoagulation in endometriomas and benign ovarian cysts: a systematic review and meta-analysis. J Assist Reprod Genet. 2024;41(10):2727-2738.
doi pubmed - Mohamed AA, Al-Hussaini TK, Fathalla MM, El Shamy TT, Abdelaal, II, Amer SA. The impact of excision of benign nonendometriotic ovarian cysts on ovarian reserve: a systematic review. Am J Obstet Gynecol. 2016;215(2):169-176.
doi pubmed - Ding Y, Yuan Y, Ding J, Chen Y, Zhang X, Hua K. Comprehensive assessment of the impact of laparoscopic ovarian cystectomy on ovarian reserve. J Minim Invasive Gynecol. 2015;22(7):1252-1259.
doi pubmed - Liang Y, Liu J, Yu Y, Sun J, Yang S, Zhang J. Effect of barbed suture versus conventional suture in laparo-endoscopic single-site cystectomy for ovarian mature cystic teratoma: An ambispective cohort study. Int J Gynaecol Obstet. 2023;161(1):93-99.
doi pubmed - Kitajima M, Khan KN, Hiraki K, Inoue T, Fujishita A, Masuzaki H. Changes in serum anti-Mullerian hormone levels may predict damage to residual normal ovarian tissue after laparoscopic surgery for women with ovarian endometrioma. Fertil Steril. 2011;95(8):2589-2591.e2581.
doi pubmed - Iwase A, Hirokawa W, Goto M, Takikawa S, Nagatomo Y, Nakahara T, Manabe S, et al. Serum anti-Mullerian hormone level is a useful marker for evaluating the impact of laparoscopic cystectomy on ovarian reserve. Fertil Steril. 2010;94(7):2846-2849.
doi pubmed - Kim YJ, Cha SW, Kim HO. Serum anti-Mullerian hormone levels decrease after endometriosis surgery. J Obstet Gynaecol. 2017;37(3):342-346.
doi pubmed - Lind T, Hammarstrom M, Lampic C, Rodriguez-Wallberg K. Anti-Mullerian hormone reduction after ovarian cyst surgery is dependent on the histological cyst type and preoperative anti-Mullerian hormone levels. Acta Obstet Gynecol Scand. 2015;94(2):183-190.
doi pubmed - Amooee S, Gharib M, Ravanfar P. Comparison of anti-mullerian hormone level in non-endometriotic benign ovarian cyst before and after laparoscopic cystectomy. Iran J Reprod Med. 2015;13(3):149-154.
pubmed - Huang BS, Wang PH, Tsai HW, Hsu TF, Yen MS, Chen YJ. Single-port compared with conventional laparoscopic cystectomy for ovarian dermoid cysts. Taiwan J Obstet Gynecol. 2014;53(4):523-529.
doi pubmed - Li H, Yan B, Wang Y, Shu Z, Li P, Liu Y, Wang Y, et al. The optimal time of ovarian reserve recovery after laparoscopic unilateral ovarian non-endometriotic cystectomy. Front Endocrinol (Lausanne). 2021;12:671225.
doi pubmed
This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (CC BY 4.0), which permits unrestricted use, distribution, and reproduction in any medium, including commercial use, provided the original work is properly cited.
Journal of Medical Cases is published by Elmer Press Inc.